May 22, 2026 – The Caribbean Community is warning that the escalating conflict surrounding the Strait of Hormuz is now directly threatening Caribbean economies, driving up the cost of fuel, food and freight across a region heavily dependent on imports.
In a statement issued this week, CARICOM expressed “serious concern” over the worsening hostilities in the Middle East and the growing instability affecting one of the world’s most critical shipping corridors.
instability affecting one of the world’s most critical shipping corridors.
CARICOM said it is alarmed by: “the severe loss of life, threats to civil infrastructure, and the instability in global markets” resulting from the conflict.
The regional bloc warned that disruption in maritime transit through the Strait of Hormuz is reverberating across the global economy through: “energy markets, supply chains and increased freight costs.”
For Caribbean citizens, those consequences are already becoming painfully visible.
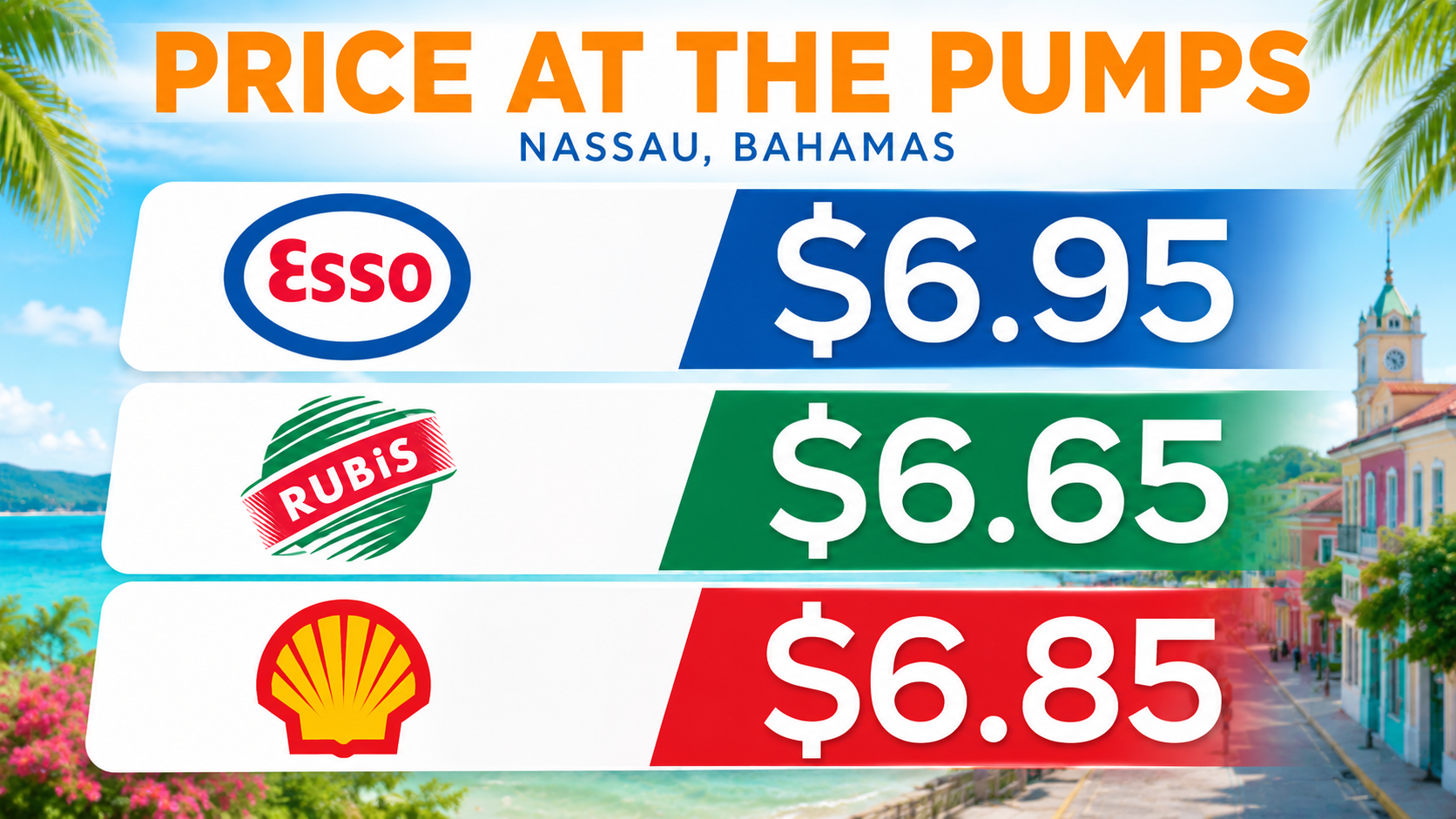
In Nassau, gasoline prices have surged again, with regular fuel now nearing or exceeding seven dollars per gallon at some stations. Consumers in other CARICOM countries are also reporting higher transportation costs, rising grocery bills and mounting pressure on household budgets.
The fear among regional leaders is that the crisis is far from over.
Roughly 20 percent of the world’s oil and liquefied natural gas normally passes through the Strait of Hormuz, making it one of the most strategically important waterways in global trade. Analysts warn prolonged disruption could trigger even higher global inflation and deeper supply chain instability.
The United Nations Food and Agriculture Organization has now warned that the crisis could become a: “systemic agrifood shock” capable of triggering a severe global food price crisis within six to twelve months.
The Caribbean is especially vulnerable because of its dependence on imported fuel, imported food and imported manufactured goods.
A recent UN regional analysis warned that shockwaves from the Middle East conflict are already reaching Caribbean nations, where rising oil prices and freight costs are increasing the price of imported food, electricity and transportation.
Global institutions are also sounding increasingly dire warnings.
The World Bank projects energy prices could surge by 24 percent this year because of the conflict, while fertilizer prices may jump by more than 30 percent — increases likely to feed directly into higher food costs worldwide.
than 30 percent — increases likely to feed directly into higher food costs worldwide.
The International Monetary Fund has meanwhile warned the global economy could face a “much worse outcome” if the conflict drags into 2027 and oil prices continue climbing.
CARICOM is now calling for all parties to respect international law and preserve safe passage through the Strait of Hormuz under the United Nations Convention on the Law of the Sea.
The Community stressed that transit passage: “should not be contingent on any license, levy, or authorization,” and warned that bordering states should not “hamper or suspend” the movement of vessels through the corridor.
CARICOM also called for: “cessation of hostilities” and urged “de-escalation and restraint by all parties.”
But for many Caribbean citizens, the economic pain is already here.
And with fuel nearing seven dollars per gallon in parts of The Bahamas, regional governments are facing renewed pressure over cost of living concerns, inflation and the Caribbean’s continued dependence on imported energy and food supplies.
Angle by Deandrea Hamilton. Built with ChatGPT (AI). Magnetic Media — CAPTURING LIFE.


 Bahamas News7 days ago
Bahamas News7 days ago
 Caribbean News7 days ago
Caribbean News7 days ago
 Caribbean News1 week ago
Caribbean News1 week ago
 News1 week ago
News1 week ago
 Caribbean News1 week ago
Caribbean News1 week ago
 Bahamas News7 days ago
Bahamas News7 days ago
 Bahamas News4 days ago
Bahamas News4 days ago
 News1 week ago
News1 week ago